Can You Have a Low Temp With Covid
- Research Alphabetic character
- Open Access
- Published:
Torso temperature correlates with mortality in COVID-19 patients
Critical Care book 24, Article number:298 (2020) Cite this commodity
Systemic inflammation that accompanies acute respiratory distress syndrome in COVID-19 [1] is associated with a high mortality rate, every bit high as 32.five% [two]. Treatment options for severe cases remain express [3]. The high mortality rate, lack of effective therapies, and extremely high volume of cases have led to a clear demand for reliable prognostic markers to indicate which patients are at the highest risk of death and thus require closer monitoring.
One gene that is common to the majority of hospitalized COVID-19 patients is fever. The degree of temperature elevation might reflect the severity of inflammation. However, there are currently no published studies that take looked at body temperature (BT) as a potential prognostic mark. We sought to analyze how BT monitoring might inform mortality rate estimates in COVID-19-positive patients.
We analyzed BT data in the de-identified database of COVID-19-suspected patients in Mountain Sinai and its affiliated hospitals in the New York area as of May 3, 2020. A full of 9417 patients tested positive for the SARS-CoV-2 virus past RT-PCR detection. After excluding patients with missing temperature data (n = 1802), 7614 patients were included in the analysis (Table one). Fifty per centum had a BT > 37 °C on the initial presentation and 78.v% of patients developed BT > 37 °C during the grade of the disease. The overall bloodshed was 16.9% with a median of 7 days to death from the initial presentation. As shown in Fig. 1a, higher BT at the initial presentation did non show a significant clan to bloodshed. Chiefly, patients presenting with BT ≤ 36 °C had the highest mortality (26.5%, P = 0.003 relative to 36 °C < BT ≤ 37 °C), and this became even higher when the analysis was restricted to those with BT ≤ 35.5 °C (44%), indicating low body temperature at the initial presentation is a marking of poor prognosis. Meanwhile, maximum BT during COVID-19 infection was significantly correlated with mortality rate (Fig. 1b). There was a significant increase in bloodshed for every 0.v °C increase in BT, and the mortality was every bit loftier as 42% in those with maximum BT > 40.0 °C.
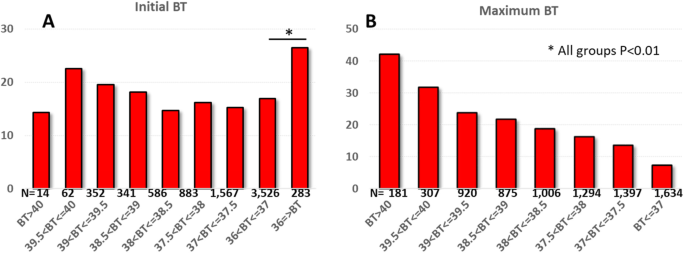
Body temperature and mortality in COVID-19 patients. a High body temperature at the initial presentation did not correlate significantly with bloodshed. Patients with BT ≤ 36 °C had significantly higher mortality compared to normothermia patients. b In that location was a pregnant increase in bloodshed for every 0.5 °C increase in maximum BT during the grade of COVID-19 (Holms test)
Our results indicate that just half of the patients with positive SARS-CoV-2 virus present with BT > 37 °C at the initial presentation. However, temperature top is common, and loftier maximum temperature during the class of SARS-CoV-2 infection was a significant straw of poor outcomes. In fact, i in iii patients reaching a maximum BT above 39.five °C died. This was approximately a 5-fold increment in mortality charge per unit every bit compared to patients whose temperature never bankrupt 37 °C. In contrast, almost one-half of the patients initially presenting with low BT (< 35.5 °C) died. Our results, therefore, suggest that poor BT control during the COVID 19 disease course is a mark of poor prognosis and BT can exist used as an easily obtained prognostic indicator.
Information technology remains unknown if controlling the high temperature in severely sick COVID-xix patients would alleviate inflammatory response and meliorate their consequence. Future studies are necessary to address this question. We acknowledge the limitations of our study including unknown methods of temperature measurement, lack of follow-up of temperature in patients without hospital admission, and that the data is not adjusted for potential confounding factors. Nevertheless, a clear tendency in increased mortality amidst the patients with poor temperature control highlights the usefulness of this non-invasively and hands obtained parameter for evaluating patients' prognoses.
Availability of data and materials
The datasets generated and/or analyzed during the current written report are non publicly available due to institutional policy but are available from the respective writer on reasonable request.
Abbreviations
References
-
Huang C, Wang Y, Li X, et al. Clinical features of patients infected with 2022 novel coronavirus in Wuhan, China. Lancet. 2020;395(10223):497–506.
-
Li X, Xu South, Yu K, et al. Risk factors for severity and bloodshed in developed COVID-19 inpatients in Wuhan. J Allergy Clin Immunol. 2020;S0091-6749(20):30495–iv.
-
Cunningham Ac, Goh HP, Koh D. Treatment of COVID-19: old tricks for new challenges. Crit Care. 2020;24(1):91.
Funding
This work was supported by NIH R01 HL139963 (KI) and AHA-SDG 17SDG33410873 (KI).
Writer information
Affiliations
Contributions
ST, KN, and KI conceived and designed the written report. ST, SM, and KI analyzed and interpreted the data. ST and KI drafted the manuscript. All authors revised the manuscript. All authors canonical the final version of the manuscript and agreed to authorship contributions.
Corresponding author
Ethics declarations
Ideals blessing and consent to participate
The IRB at the Icahn Schoolhouse of Medicine at Mount Sinai reviewed the data collection protocol and deemed scientific publication of the de-identified patient data exempt from the IRB review.
Consent for publication
Not applicative.
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher's Annotation
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open up Access This article is licensed under a Creative Eatables Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in whatever medium or format, as long equally you lot give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and signal if changes were made. The images or other tertiary party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the fabric. If textile is non included in the article's Creative Commons licence and your intended apply is not permitted by statutory regulation or exceeds the permitted apply, you volition need to obtain permission straight from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/aught/i.0/) applies to the information fabricated bachelor in this article, unless otherwise stated in a credit line to the data.
Reprints and Permissions
Near this article
Cite this article
Tharakan, S., Nomoto, K., Miyashita, S. et al. Torso temperature correlates with mortality in COVID-19 patients. Crit Intendance 24, 298 (2020). https://doi.org/10.1186/s13054-020-03045-eight
-
Received:
-
Accepted:
-
Published:
-
DOI : https://doi.org/10.1186/s13054-020-03045-8
Source: https://ccforum.biomedcentral.com/articles/10.1186/s13054-020-03045-8
0 Response to "Can You Have a Low Temp With Covid"
Post a Comment